By Duan Xingyu, Shao Huizhen, Ren Zhongqi
Introduction
In 2015, the United Nation included “Good Health and Wellbeing” as one of the 17 sustainable development goals, which has set up a higher threshold for the construction of public health and health-care facilities. Yet in 2020, COVID-19 has posed a massive challenge to the health-care system of the whole world, in which a great number of them have collapsed, including those on the continent of Africa.
Despite a distinct advantage in the fightback against the COVID-19 pandemic owing to relatively high temperatures throughout the year, the number of infected cases and the death toll have never stopped rising. In contrast, Uganda—a country located in Eastern Africa with a population of 4.2 million people—managed to keep the outbreak under control.
In this article, key indicators reflecting the trends of the pandemic in Uganda were collected, and the data are presented in figures plotted by R. With these figures, we aim to analyze the factors contributing to the trend of the pandemic in Uganda and the approach which Uganda government applied to respond to the outbreak of the virus. Finally, the case of prevention and the control of the COVID-19 in Uganda will be evaluated and lessons learned from the case will be illustrated.
How Does the Pandemic Develop in Uganda

Fig.1 presents the trends of new cases in East African countries from March 2020 to February 2021. Despite fewer cases identified and smaller peaks of the outbreak, the curve of Uganda still follows the trend of East African countries, especially its close neighbor, Kenya. From February to August 2020, the pandemic was well controlled compared to other countries in East Africa. In August, the number of new cases slightly increased but soon slumped. In November 2020, the country, following the pace of Kenya, was struck by a more serious outbreak. The massive outbreak didn’t calm down until January 2021 when the number of new cases declined.
Compared to Fig.1, the reproduction rate (R number) in Fig.2 illustrates the issue with more details. Reproduction rate, representing the mutation rate and toxic strength (transmission intensity) of an infectious virus, is the proportion of the people who are reinfected after they have been cured of the infection or have gotten the vaccination (including those who may have been infected with new coronavirus or have gotten the vaccination). The reproduction rate of COVID-19 in Uganda reached the top in August 2020 and fluctuated in October and November. From November to January 2021, the Reproduction rate decreased constantly.

Government Response and Other Contributing Factors
The government of Uganda had implemented some effective measures to prevent and control the spread of the pandemic, which set the country apart from its neighbor.
First of all, by releasing a series of guidelines, the government tried to educate the public and restricted mass gathering, and standardized the prevention measures on various occasions including the market, working places, and prison at the beginning of March when the pandemic had not yet extended its formal greetings to the country. [2][3]
On March 21st, the first case was identified in Uganda. The government responded instantly by releasing a series of documents, stipulating that entry into the country, cargo or people, were prohibited, and the stores and markets were shut down to minimize the circulation domestically. [4][5] The provisions also included curfews, limits on transportation, and so on. [4][5] By doing this, the transmission modes of the virus were restricted, so the pandemic in Uganda didn’t show an outbreak in April compared with its neighbor in East Africa.
These measures prepared the country for the pandemic battle and also played a vital role in pandemic control at the early stage. Until the beginning of August, the curve of new cases per day didn’t show a sharp increase. Overall, Uganda built a sensitive sentinel surveillance so that it can respond as soon as possible when an emergency happens, which made Uganda’s incidence rate fluctuate marginally in May 2020. As predicted, the reproduction rate has moderate peaks and troughs before the surge in August, and the positive rate stands at a low level because of the steady incidence rate.
After a series of effective and in-time respondents, the increased curve and death rate of this new virus was not as high as citizens were expecting. They were hesitant in spending their money on the prevention supplies. Many of the public refused to wear masks even in public places. [1] At the same time, the lockdown and closure policy was chosen to be ceased to reduce the heavy burden on the economy. The circulation of cargo and people came hand in hand with the spread of the pandemic where prevention inside the country was not performed as expected. Therefore, the incidence rate mounted in August and November, and the reproduction rate multiplied in August.
Besides the cease of strong policy, the surge of incidence rate may also be attributed to the widespread new variants. According to a study published on Nature[8], researchers sequenced more than 1,300 new coronavirus which was isolated in South Africa during the last six months and found 13 different variants in total. Based on the study, it’s evident that the newly discovered C series variant, especially C.1 is the most widely spread variant in South Africa in August, which may take the responsibility for the surge of the reproduction rate in Uganda.
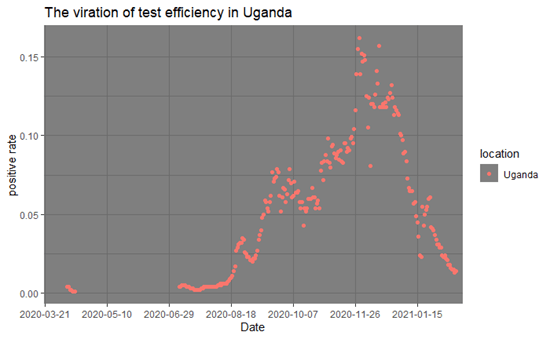
Though the measures that directly controlled the spread of the virus were, to some extent, short-term ones, other efforts were also made by the government to strive for the balance between limited medical resources and the need of controlling the pandemic. To increase the efficiency of the medical system, the government issued guidelines to standardize the procedure of diagnosis and treatment. They also tried to set up places for quarantine and specify the measures for treating HIV and TB against the background of COVID-19. [6] In August, the government shrank its payment on tests to release the fiscal burden and save insufficient test kits. This stipulation declared that the government only provided free tests for the suspected infected, the contacts, the infected, and front-line health workers, while other people should pay for the tests themselves. [7] Though narrowing the coverage of tests, the stipulation increased the efficiency of testing. From September 1st when the policy came into effect, the positive rates of tests which signifies the proportion of the infected in the total tests, showed a continued growth which can be seen in Fig.3.
Summary of the Issue
The Uganda government, with the help of the international community, has tried its best in educating the public, standardizing the diagnosis and treatment procedure, preventing and controlling the spread of the virus, and coordinating the medical resources with proper policies. With strong policies, the increase in the number is slow compared with other countries in East Africa. However, limited policies only served to cope with the emergency. Given the downturn in the economy, with no long-term measures taking place, the country has experienced severe disruption of essential health services and loss of human capital accumulation.
Lessons Learned
The inefficiency tells that input into public health and improving the health system is still a priority for Uganda. To do this, the government may first record and tidy the resources being used in the battle against COVID-19. It is recommended that the government help record the health workers who haven’t registered in the office, and establish more fundamental equipment based on the ones that are temporarily employed during the pandemic time. By doing this, the resources can be integrated as part of the prevention and control system for infectious diseases. What’s more, the government needs to have a viable plan of health system strengthening and resource
enriching the medical resources for the long run.
Reference
[1]Shanggai Academy of Global Governance & Area Studies. Dynamic reporting of new coronavirus outbreaks in East Africa[EB/OL].
http://www.saggas.shisu.edu.cn/Detail.aspx?id=1.325,2020-06-10/2021-03-05
[2]Republic of Uganda. Guidelines for Prevention of COVID-19 in Markets. Kampla: Ministry of Health [EB/OL]. https://covidlawlab.org/?s=&topic=®ion=&country=Uganda&type=&sorting=date_issued&tag=,2020-03-01/2021-03-05
[3] Republic of Uganda. COVID19 Guidelines on Mass Gatherings. Kampla: Ministry of Health[EB/OL]. https://covidlawlab.org/?s=&topic=®ion=&country=Uganda&type=&sorting=date_issued&tag=,2020-03-01/2021-03-05
[4] Republic of Uganda. The Public Health (Control of COVID-19) (No.2) RULES, 2020. Kampla: Ministry of Health[EB/OL]. https://covidlawlab.org/?s=&topic=®ion=&country=Uganda&type=&sorting=date_issued&tag=,2020-03-31/2021-03-05
[5] Republic of Uganda. Public Health (Control of COVID-19) Rules, 2020. Kampla: Ministry of Health[EB/OL]. https://covidlawlab.org/?s=&topic=®ion=&country=Uganda&type=&sorting=date_issued&tag=,2020-03-24/2021-03-05
[6] Republic of Uganda. COVID19 Guidance for HIV and TB Services[EB/OL]. https://covidlawlab.org/?s=&topic=®ion=&country=Uganda&type=&sorting=date_issued&tag=,2020-04-16/2021-03-05
[7] Republic of Uganda. User fees policy for COVID-19 testing in Uganda. Kampla: Ministry of Health[EB/OL]. https://covidlawlab.org/?s=&topic=®ion=&country=Uganda&type=&sorting=date_issued&tag=,2020-08-27/2021-03-05
[8]Houriiyah Tegally,Eduan Wilkinson,Richard J.Lessells etc.Sixteen novel lineages of SARS-CoV-2 in South Africa[J/OL].Nature.2021-02/2021-03-05
[9] Republic of Uganda. Updated response to Sunday monitor article on cost of covid-19 tests by permanent secretary[EB/OL]. https://www.health.go.ug/cause/updated-response-to-sunday-monitor-article-on-cost-of-covid-19-tests-by-permanent-secretary/,2020-09-24/2021-03-05


